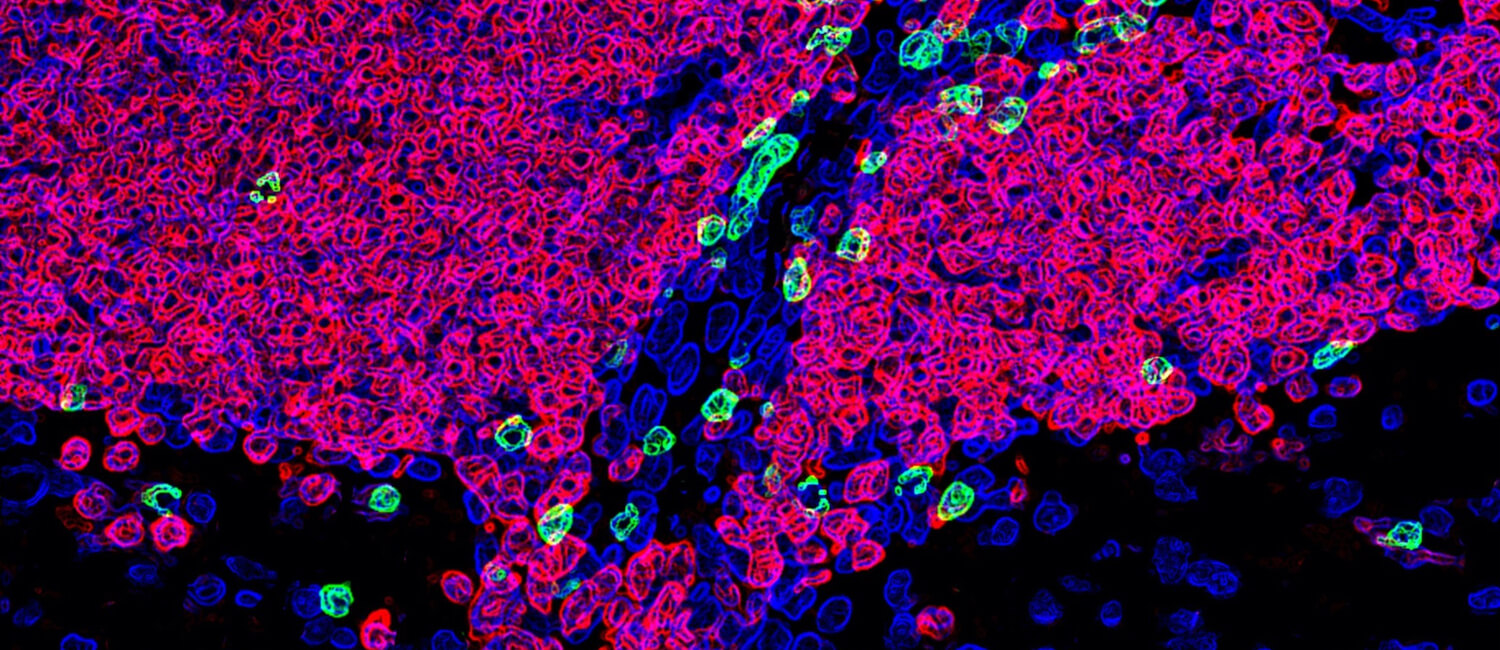
 A naturally occurring canine disease called granulomatous meningoencephalomyelitis replicates many features of multiple sclerosis, including the involvement of B cells (in red) and T cells (green)
A naturally occurring canine disease called granulomatous meningoencephalomyelitis replicates many features of multiple sclerosis, including the involvement of B cells (in red) and T cells (green)
in the tissues that line the central nervous system.
The canine disease granulomatous meningoencephalomyelitis (GME), the most common neuroinflammatory disease that affects dogs, shares key features of its pathology and immunology with multiple sclerosis (MS), according to a new study.
 Dr. Jorge Alvarez
Dr. Jorge Alvarez
A detailed investigation of GME by a team led by Molly Church and Jorge Iván Alvarez of Penn’s School of Veterinary Medicine, incorporating MRI images and studies of brain tissue, found that defining characteristics of MS—notably the accumulation of B cells in the tissues that line the central nervous system—were also present in dogs with GME. B cells are a type of white blood cell involved in immune responses. In healthy people, such immune cells are present in very low numbers in the membranes that line the spine and brain, known as the meninges. The team reported its findings in the Journal of Immunology.
“That’s a novel aspect of the disease in dogs that is mirroring the pathology in humans,” says Alvarez. “And it’s something that people are not able to replicate in mouse models of MS. We feel that by studying dogs with GME, we can expand knowledge of a human disease and contribute to the pressing need to understand the disease in dogs as well.”
 Dr. Molly Church
Dr. Molly Church
“We looked at these accumulations of B cells in the dogs’ meninges and saw striking similarities to MS. Those specific accumulations in the meninges overlying the cerebrum has never been looked at in GME dogs,” says Church. “Describing this new component of GME that hadn’t yet been considered could lead the way to better diagnostics, as well as better therapeutics to augment what is already in use.”
Nearly a million people in the United States are living with MS. The disease is characterized by gradual destruction of the protective lining of nerve cells, leading to a wide array of possible symptoms, from vision problems to pain to fatigue. Severity can range from patient to patient. Yet despite its prevalence, MS remains somewhat a mystery. It’s only been intensively studied since the 1970s, and sometimes proves difficult to diagnose. While a dozen or more approved drugs exist to treat its relapsing-and-remitting forms, treating its more advanced, progressive forms has proved challenging.
Similarly, GME is a disease that has only been characterized in the past few decades and is generally diagnosed by exclusion of other diseases. While some dogs respond well to immunosuppressive treatment, others briefly stabilize clinically, and still others decline rapidly following diagnosis.
Both MS and GME are more common in females and tend to affect young and middle-aged patients.
In MS, a high degree of inflammation was linked with poorer outcomes, and it was believed that T cells, another immune cell type, were to blame.
“Most drugs developed in the ‘90s and 2000s were aiming at those cell types,” says Alvarez. “It’s only in the last 10 years or so that people have come to recognize that B cells play a role.” Given the important function of B cells in MS, Alvarez and Church collaborated with Amit Bar-Or, chief of the MS & Related Disorders Center at Penn’s Perelman School of Medicine. He is an expert on B cells who brings the perspective of the human disease to these findings.
Advancements in MS research has been impeded in part by the lack of animal models that faithfully replicate the involvement of B cells in the disease, the researchers say, motivating a closer look at GME.
Embedded in the very name of the disease, granulomatous is a belief that macrophages, a component of the innate immune system that responds to infection and can result in inflammation, were the primary cultprits in causing harm. But in the new study, Alvarez, Church, and colleagues looked deeper.
In 13 dogs diagnosed with GME, as well as four unaffected dogs, Church, a pathologist, examined areas of the brain typically not looked at during GME diagnosis. MRI images analyzed by Penn Vet’s Charles Vite showed increased contrast in the meninges. When assessing the corresponding tissue from the dogs, they found accumulations of inflammatory cells, and of B cells, specifically, in those areas.
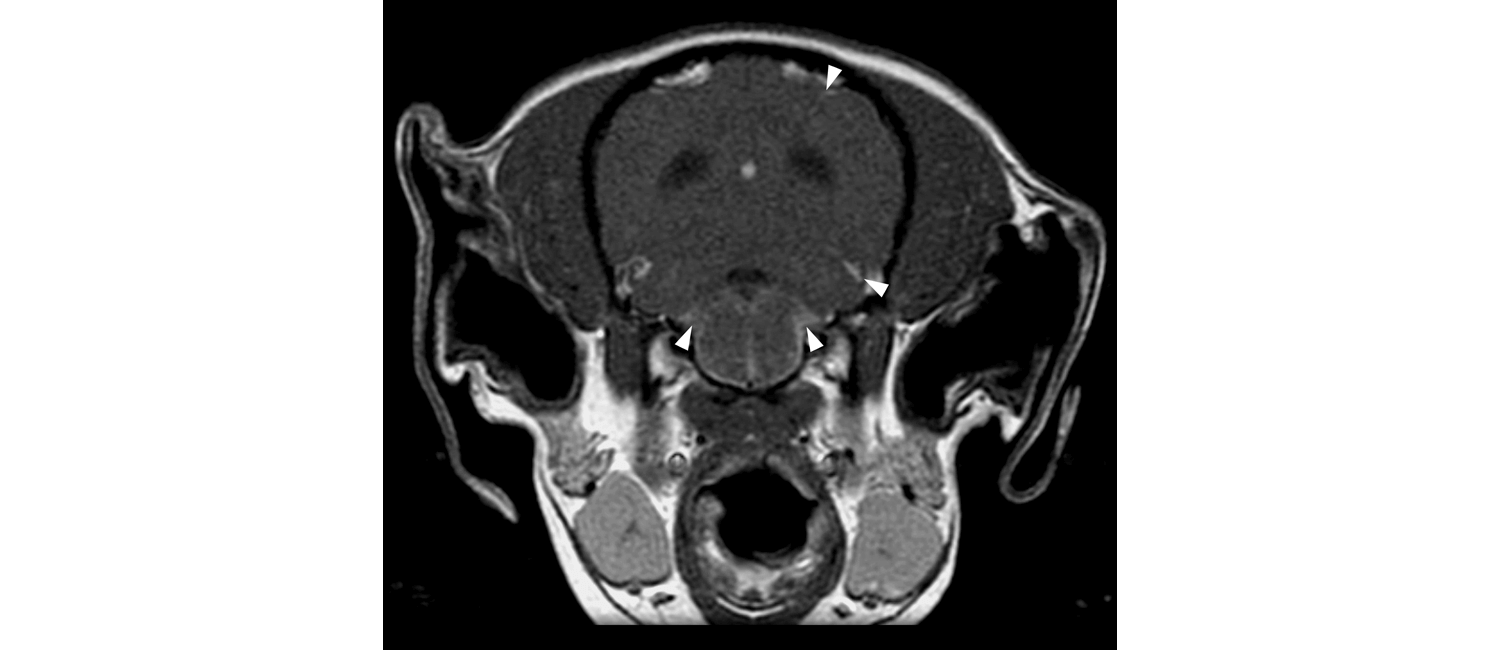 A dog with GME has areas of higher contrast (indicated by arrows) in the meninges, where B cells accumulate.
A dog with GME has areas of higher contrast (indicated by arrows) in the meninges, where B cells accumulate.
This is also seen in chronic forms of multiple sclerosis.
Alvarez’s lab, which focuses on the link between central nervous system inflammation and MS, evaluated the components of these inflamed regions of the meninges and found an accumulation of B cells.
“In humans it has been shown that those collections of B cells correlate with underlying pathology in the brain,” Alvarez says, “And we observe the same feature in GME. That’s why we believe that this model holds great potential.”
The fact that dogs and humans often share an environment and that the biology of dogs is more similar to humans than the mice often used in preclinical MS studies adds to the value of studying GME as a model of MS, the researchers note.
“We can all learn from studying this disease in dogs,” says Church, “certainly as a model for human disease, but the wonderful thing that can come out of comparative studies like this is that we not only help people, we help our canine patients as well.”
Jorge Iván Alvarez is an assistant professor of pathology in the University of Pennsylvania School of Veterinary Medicine. He also held the David L. Torrey EndMS transitional career development award from the Multiple Sclerosis Society of Canada.
Molly E. Church is an assistant professor of pathology in Penn’s School of Veterinary Medicine.
Alvarez and Church’s coauthors are Guadalupe Ceja, Megan McGeehan, Miles C. Miller, Priscilla Farias, Melissa D. Sánchez, Gary P. Swain, Charles-Antoine Assenmacher, and Charles H. Vite of Penn Vet; Amit Bar-Or of the Universtiy of Pennsylvania Perelman School of Medicine; and Edward G. Stopa of Brown University.
This study has been supported by the the National Institutes of Health by grants NINDS 5K01NS097519-03 and NCATS 5UL1TR001878-04 to the Institute of Translational Medicine and Therapeutics and via the Program in Comparative Animal Biology of the University of Pennsylvania.