Major projects in the laboratory include:
Defining a role for type III Collagen (Col3) in regenerative and tumor microenvironments
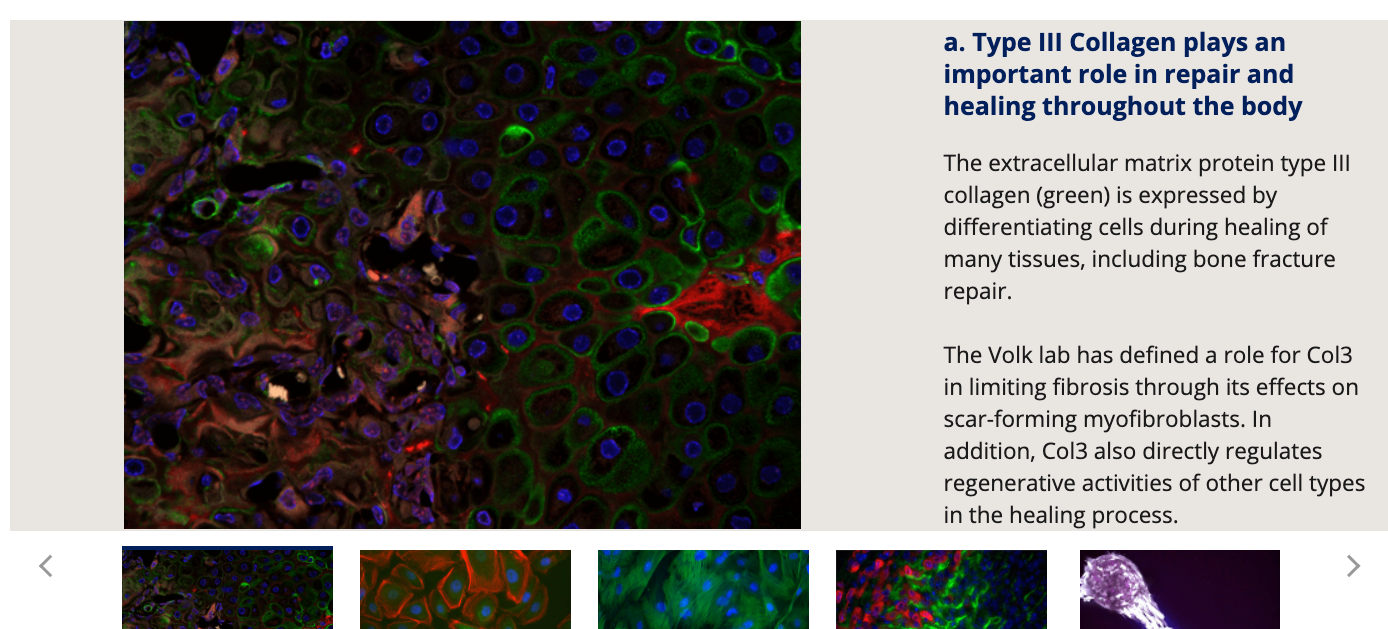
Our publications have characterized a key role for Col3 in directing cellular activities and fate in regenerative and tumor microenvironments.
Although Col3 has been widely speculated to play a role in wound healing due to its temporospatial pattern of expression following injury, our studies were the first to reveal a role for Col3 in 1) regulating reepithelialization and scar formation during cutaneous wound healing and 2) modulating bone formation during development and fracture repair. These studies have important implications for the development of novel strategies to target major medical issues such as chronic non-healing wounds, disorders of excessive scar formation, impaired bone healing and osteoporosis. Our study showing that Col3-deficiency promotes scar deposition through the promotion of myofibroblast density and persistence following injury has led to a paradigm shift in the understanding of how individual collagens can suppress scar formation/fibrosis rather than simply contributing to the process. Ongoing studies seek to define mechanisms by which Col3 regulates cell activities and fate and apply this knowledge to the development of novel biomaterials for tissue engineering strategies.
As tumors have been referred to as “wounds that do not heal”, our recent publication identifying a role for Col3 in suppressing breast cancer growth and metastasis by its ability to direct stromal organization complements our wound healing studies. Current studies will determine mechanisms by which Col3 regulates the switch between a tumor-restrictive and tumor-permissive stroma and address the hypothesis that Col3-based regenerative strategies can effectively limit recurrence of certain cancers.
Regenerative therapies for cutaneous wound healing
The extremes in response to cutaneous injury, both non-healing chronic wounds and pathologic scar formation, are a significant cause of morbidity and health care expenditures. Together with collaborators, our laboratory has shown regenerative medical strategies (cell-based therapies, electrical stimulation and biomaterials) improve quality of cutaneous wound healing, and determined mechanisms by which they promote optimal repair, using small and large animal models as well as in human subjects.
Cellular-based therapies to improve tissue repair in canine models
Our laboratory has a long-standing interest in adult cell-based therapies, with a goal to develop and then optimize novel treatments to improve healing of companion animals. Studies in my laboratory have focused on advancing a thorough, systematic understanding of the basic biology of canine MSCs to inform the design of future stem cell clinical trials in the dog and their use for translational studies. As spontaneous large animal models play a key role in defining efficacy of regenerative medical therapies, these early studies have provided critical data for model development. Our current clinical trial in client-owned dogs with elbow dysplasia will compare efficacy of post-operative cell-based therapies (bone marrow vs adipose-derived) in improving clinical outcomes.
Stromal targets in cancer of companion animals
Studies from a large number of laboratories, including our own, have revealed a critical role for the tumor stroma in controlling cancer behavior. As aggressive stromal signatures predict metastasis and survival in both murine breast cancer models and human patients, we predict these signatures may provide similar prognostic information in dogs and cats with mammary gland tumors. Mammary gland tumors, the most common malignancies in intact female dogs and the third most common in female cats, represent a significant canine health problem. Two major obstacles limit our care of dogs and cats with mammary carcinoma: 1) accurate identification of patients at high-risk of local recurrence and/or metastasis and 2) effective therapies for at risk individuals.
In collaboration with Dr. Karin Sorenmo, Director of the Penn Vet Shelter Canine Mammary Tumor Program, and Dr. Ellen Pure, Director, Penn Vet Cancer Center, University of Pennsylvania School of Veterinary Medicine and an internationally-recognized expert in the field of the tumor microenvironment, our ongoing studies aim to:
- Identify stromal signatures that predict recurrence/clinical outcomes in dogs and cats with mammary gland tumors to avoid over-treatment of low-risk patients as well as under-treatment of those that require early, aggressive intervention
- Determine mechanisms driving formation of a tumor permissive stroma
- Develop safer, more effective therapies for patients with mammary tumors
Although our initial studies have focused on canine mammary tumors, we have also begun applying our findings to cancers in cats as well. As spontaneously occurring canine and feline mammary carcinomas share many similarities with human breast cancer, our findings may have direct application to human breast cancer research, thus helping both dogs, cats, and women with breast cancer.
The Volk Laboratory comprises a team of senior faculty, post-doctoral fellows, PhD candidates, students, and technicians.


Dr. Susan W. Volk, Named Corinne R. and Henry Bower Professor of Surgery at Penn Vet (Dec. 9, 2019): Volk is an international thought leader, speaker, and inventor. Her current research funding includes two NIH grants (RO1) as PI, along with other private foundation awards. Her body of research focuses on mechanisms by which the extracellular matrix regulates key processes in the wound healing-fibrosis-cancer triad. Dr. Volk’s awards include the Penn Center for Innovation’s 2019 Emerging Inventor of the Year and the Wound Healing Foundation’s 2021 Translational Regenerative Science Award. She is a member of the Editorial Board of Wound Repair and Regeneration and an elected member of the Board of Directors for both the Wound Healing Society and the North American Veterinary Regenerative Medicine Association. Recently elected vice president of the Wound Healing Society, Volk will assume the Society’s presidency in 2025. Read More

Congratulations to Dr. Daniel Stewart, postdoctoral fellow in the Volk Laboratory, on winning the Young Investigator Award at the 2023 Wound Healing Society Meeting!

Emerging Inventor of the Year Award (Dec. 9, 2019): Dr. Susan Volk recently received the Emerging Inventor of the Year Award from the Penn Center for Innovation. Volk’s research program focuses on the reciprocal, dynamic interactions of stem and progenitor cells with the extracellular matrix, and the role progenitor and reparative cells have in regulating normal and pathological healing as part of the triad of wound healing, fibrosis, and cancer. She has identified the mechanisms by which type III collagen (Col3) promotes a regenerative response following cutaneous injury, as well as her discovery that Col3 directs stromal organization and limits metastasis in a murine model of breast cancer. Volk has also recently identified predictive collagen signatures and potential therapeutic targets in canine mammary tumors.
Dr. Volk's research was featured in Penn News.Read the full article:
- Brisson BK, Stewart DC, Burgwin C, Chenoweth D, Wells RG, Adams SL, Volk SW*. Cysteine-rich domain of type III collagen N-propeptide inhibits fibroblast activation by attenuating TGFb. Matrix Biology.2022; 109: 19-33. doi: 10.1016/j.matbio.2022.03.004.PMID: 35339637. PMCID: PMC9086147.
- Terajima M, Taga Y, Brisson BK, Durham AC, Sato K, Uzawa K, Saito T, Hattori S, Sørenmo KU, Yamauchi M*, Volk SW*.Collagen molecular phenotypic switch between non-neoplastic and neoplastic canine mammary tissues.Sci Reports.2021; 11(1): 8659.Doi: 10.1038/s41598-021-87380-y.PMID:33883562.PMCID:PMC8060395.
Bonnevie ED, Ashinsky BG, Dekky B, Volk SW, Smith HE, Mauck RL. Cell morphology and mechanosensing can be decoupled in fibrous microenvironments and identified using artificial neural networks. Sci Reports. 2021 Mar 15;11(1):5950. doi: 10.1038/s41598-021-85276-5. PMID: 33723274.PMCID:PMC7961147.
- Witherel CE, Sao K, Brisson BK, Han B, Volk SW, Petrie RJ, Han L, Spiller KL. Regulation of extracellular matrix assembly and structure by hybrid M1/M2 macrophages. Biomaterials. 269:120667. doi: 10.1016/j.biomaterials.2021.120667. PMCID: PMC7870567.
- Rosen SG, Brisson BK, Durham AC, Munroe CM, McNeill CJ, Stefanovski D, Sorenmo KU, Volk SW*. Intratumoral collagen signatures predict clinical outcomes in feline mammary carcinoma.PLoS One,15(8): e0236516 doi: 10.1371/journal.pone.0236516, 2020. PMCID: PMC7416937.
- Wang C, Brisson BK, Terajima M, Li Q, Hoxha K, Han B, Goldberg AM, Liu S, Macrolongo MS, Enomoto-Iwamoto M, Yamauchi M, Volk SW*, Han L*. Type III Collagen is a Key Regulator of the Collagen Fibrillar Structure and Biomechanics of Articular Cartilage and Meniscus, Matrix Biology, 85-86:47-67. doi: 10.1016/j.matbio.2019.10.001, 2020. PMCID: PMC7137252.
- Ortiz A, Gui J, Zahedi F, Bhattacharya S, Carbone CJ, Yu Q, Katlinski KV, Katlinskaya YV, Handa S, Haas V, Volk SW, Brice AK, Wals K, Matheson NJ, Ludwig S, Whiteside TL, Sander C, Tarhini AA, Kirkwood JM, Lehner PJ, Rui H, Minn AJ, Koumenis C, Diehl JA, and Fuchs SY. An oxysterol-based defense against the tumor-derived extracellular vesicles. Cancer Cell, 14;35(1):33-45.e6. doi: 10.1016/j.ccell.2018.12.001, 2019. PMCID: PMC6336114.
- Raposo-Ferreria TMM, Brisson BK, Durham AC, Laufer-Amorim R, Kristiansen V, Puré E, Volk SW*, Sørenmo KU*.Characteristics of the Epithelial-Mesenchymal Transition in Primary and Paired Metastatic Canine Mammary Carcinomas. Vet Pathology, 55(5):622-633: doi:10.1177/0300985818776054, 2018. PMCID: PMC7993492.
- Case A, Brisson BK, Durham AC, Rosen S, Monslow J, Buza E, Salah P, Gillem J, Ruthel G, Veluvolu S, Kristiansen V, Puré E, Brown DC, Sørenmo KU, Volk SW*.Prognostic collagen signatures in canine mammary carcinoma.PLOS One, 12(7): e0180448, 2017. PMCID: PMC5500345.
- Glennie ND, Volk SW, Scott P.Skin resident CD4+ T cells protect against Leishmania major by recruiting and activating inflammatory monocytes. PLOS Pathogens, 13(4): e1006349, 2017. PMCID: PMC5409171.
- Sebastian A, Volk SW, Halai P, Colthurst J, Paus R, Bayat A.Enhanced neurogenic biomarker expression and reinnervation in human acute skin wounds treated by electrical stimulation. J Invest Dermatol, 137(3):737-747, 2017.
- Wormser C, Mariano A, Holmes ES, Aronson LR, Volk SW*. Post-transplant malignant neoplasia associated with cyclosporine-based immunotherapy: prevalence, risk factors and survival in feline renal transplant recipients. Vet Comp Oncol, 14(4): e126-e134, 2016.
- Rak GD, Osborne LC, Siracusa MC, Kim BS, Wang K, Bayat A, Artis D*, Volk SW*.IL-33-dependent group 2 innate lymphoid cells promote cutaneous wound healing.J Invest Dermatol, 136 (2):487-96, 2016. PMCID: PMC4731037.
- Han Z, Bart SM, Ruthel G, Burgt NHV, Haines KM, Volk SW, Vite CH, Freedman BD, Bates P, Harty RN. Ebola virus mediated infectivity is restricted in canine and feline cells. Vet Microbiol, 182:102-7, 2016. PMCID: PMC4695692.
- Glennie ND, Yeramilli VA, Beiting DP, Volk SW, Weaver CT, Scott P.Skin Resident Memory CD4+ T Cells Enhance Protection Against Leishmania major Infection. J Exp Med, 212(9): 1405-14, 2015. PMCID: PMC4548053.
- Shen, Y-I, Song H-H, Papa A, Burke J, Volk SW, Gerecht S.Acellular hydrogels for regenerative burn wound healing: translation from a porcine model. J Invest Dermatol, 135(10): 2519-29, 2015. PMCID: PMC4570841.
- Brisson BK, Mauldin EA, Lei W, Vogel LK, Power AM, Lo A, Dopkin D, Khanna C, Wells RG, Puré E, Volk SW*. Type III collagen directs stromal organization and limits metastasis in a murine model of breast cancer. Am J Pathol. 185(5): 1471-86, 2015.PMCID: PMC4419211.
- Miedel EL, Brisson BK, Hamilton T, Gleason H, Lopas L, Dopkin D, Hankenson KD, Volk SW*.Type III collagen modulates fracture callus bone formation and early remodeling.J Orthop Res, 33(5): 675-84, 2015.PMCID: PMC4406871.
- Sebastian A, Iqbal SA, Colthurst J, Volk SW, Bayat A.Electrical stimulation enhances epidermal proliferation in human cutaneous wounds by modulating p53-SIVA1 interaction. J Invest Dermatol, 135(4): 1166-74, 2014.
- Volk SW*, Shah SR, Cohen AJ, Wang Y, Brisson BK, Vogel LK, Hankenson KD, Adams SL.Type III collagen regulates osteoblastogenesis and the quantity of trabecular bone. Calcif Tiss Intl, 94(6): 621-31, 2014. PMCID: PMC4335719.
- Volk SW*, Wang Y, Hankenson KD. Effects of donor characteristics and ex vivo expansion of canine mesenchymal stem cell properties:Implications for MSC-based therapies.Cell Transplant, 21(10): 2189-200, 2012. PMCID: PMC3840229.
- Volk SW*, Wang Y, Mauldin EA, Liechty KW and Adams SL. Diminished type III collagen promotes myofibroblast differentiation and increases scar deposition in cutaneous wound healing. Cells, Tissues, Organs 194(1):25-37, 2011. PMCID: PMC3128157.
- Peranteau WH, Heaton TE, Gu Y-C, Volk SW, Bauer TR, Alcorn K, Tuschong LM, Johnson MP, Hickstein DD and Flake AW. Haploidentical in utero hematopoietic cell transplantation improves phenotype and can induce tolerance for postnatal same donor transplants in the canine leukocyte adhesion deficiency model. Biol Blood Marrow Transpl 15: 293-305, 2009. PMCID: PMC2796507.
- Volk SW, Radu A, Zhang L and Liechty KW. Stromal progenitor cell therapy corrects the wound healing defect in the ischemic rabbit ear model of chronic wound repair. Wound Repair Reg 15: 736-47, 2007.
- Parton AT, Volk SW and Weisse C. Gastric ulceration subsequent to partial invagination of the stomach in a dog with gastric dilatation-volvulus. J Am Vet Med Assoc 228: 1895-900, 2006.
- Volk SW, Diefenderfer DL, Christopher SA, Haskins ME and Leboy PS. Effects of osteogenic inducers on cultures of canine mesenchymal stem cells. Am J Vet Res 66: 1729-37, 2005.
- Volk SW, Kapatkin AS, Haskins ME, Walton RM and D’Angelo M.Gelatinase activity in synovial fluid and synovium obtained from healthy and osteoarthritic dogs. Am J Vet Res 64:1225-33, 2003.
- Ponder KP, Melniczek JR, Xu L, Weil MA, O’Malley TM, O’Donnell PA, Knox VW, Aguirre GD, Mazrier H, Ellinwood NM, Sleeper M, Maguire AM, Volk SW, Mango RL, Zweigle J, Wolfe JH and Haskins ME. Therapeutic neonatal hepatic gene therapy in mucopolysaccharidosis VII dogs. Proc Natl Acad Sci USA99: 13102-107, 2002. PMCID: PMC130593
- Leboy P, Grasso-Knight G, D’Angelo M, Volk SW, Lian JV, Drissi H, Stein GS and Adams SL. Smad-Runx interactions during chondrocyte maturation. J Bone Joint Surg [Am] 83-A Suppl 1 (Pt1): 15-22, 2001.
- Volk SW, D’Angelo M, Diefenderfer DL and Leboy PS. Utilization of bone morphogenetic protein receptors during chondrocyte maturation. J Bone Miner Res 15: 1630-9, 2000.
- Volk SW, LuValle P, Leask T and Leboy PS. A BMP-responsive transcriptional region in the chicken type X collagen gene. J Bone Miner Res13, 1521-9, 1998.